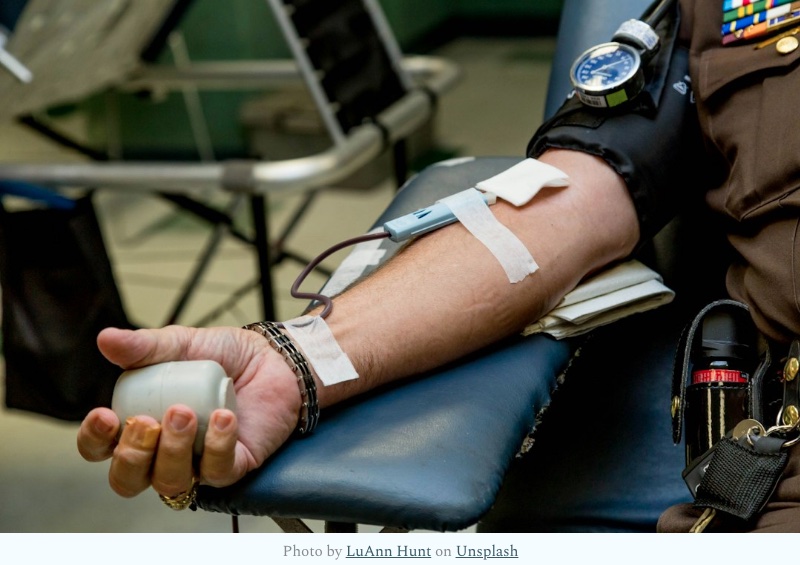
If You Can Donate Blood, You Can Help Save a Life
Have you ever given blood? If you are eligible to donate blood but haven’t, would you consider it?
Depending on a person’s size, the average adult has between 1.2 to 1.5 gallons of blood circulating throughout their body. That’s about 10 units (about a pint) of blood. Compare that with a newborn, who has only about one cup! If you, an adult, give away one of those units, you could help save up to 3 lives.
Blood donations are precious
All blood donations are precious, from the least common blood type (AB-negative) to the most common (O-positive). If you need blood, ideally, you will get your own blood type. Receiving a different one can cause serious complications. There are exceptions though , especially in an emergency. This American Red Cross page explains the four blood types (A, B, AB, and O) and why you are either positive or negative and what kind of blood your body can accept if your type is unavailable.
, especially in an emergency. This American Red Cross page explains the four blood types (A, B, AB, and O) and why you are either positive or negative and what kind of blood your body can accept if your type is unavailable.
There is no viable manufactured alternative to blood yet. However, some people who oppose blood transfusions for religious reasons (Jehovah’s Witnesses) may choose different non-blood volume expanders. If there is a blood shortage, the doctor may also give you this.
But what about O-negative blood? Medical dramas on TV often show a trauma patient wheeled into the emergency department, and someone shouts out, “Hang a unit of O neg!” Anyone with any type of blood can receive O-negative blood. People with O-negative blood are very popular during many blood drives. They are Universal Donors. Unfortunately, people with O-negative blood can only receive O-negative. They can’t tolerate any other type.
Thousands of units of blood needed daily
About 29,000 units of blood are needed across the country every day. Every two seconds, someone needs either whole blood, or one of its components such as red blood cells, plasma, or platelets. Unfortunately, hospitals can’t store blood for long. They can’t save it for later. Red blood cells have a shelf life of only six weeks. That means hospitals need a constant supply of blood, throughout the whole year. Typically, the summer season is the slowest for blood donations – people go away, they get busy, and they’re often out of their usual routine.
Donating blood
The process of donating blood is pretty easy, but not everyone should or can give. Giving blood when you’re not healthy can make you sicker. Sometimes, not being allowed to donate is a temporary situation, like when you’re sick with a cold, flu, or other viral illness; other times, it’s permanent.
This page on the Memorial Sloan Kettering Cancer Center site explains different medical conditions that affect blood donations.
In addition, your travel history is important. If you have recently traveled to countries endemic with malaria, you may be asked to wait to donate. Previous travel and residency restrictions associated with the UK, Ireland and France associated with concern for mad cow disease have now been lifted.
The blood donation process
Whether you go to a permanent blood donation center or a pop-up donation event, the blood donation process is very similar.
Registration: This is when you answer questions to make sure you’re eligible to donate. This is necessary even if you’ve donated multiple times already because they need to know what types of medications you take and your current state of health. If you have a cold or a viral infection, for example, you shouldn’t give blood. Someone will take your temperature, pulse, and blood pressure, and take a drop of blood from your finger to check your hemaglobin.
The donation: Someone will escort you to a lounge chair or cot. Someone will check the inside of your elbow to see where they will insert the needle and clean the area well. Then, using a new sterile needle, they will insert it into the vein, making sure the blood flow is consistent. Many people loosely place a piece of gauze over the needle to cover it. It usually takes about 10 minutes or so for someone to fill the donation bag. If the blood flows too slowly, squeezing a wad of paper or a ball helps. When done, the nurse or technician removes the needle. You will be asked to apply pressure to the area and wait. The whole process of filling a unit of blood takes about 10 minutes.
 When the blood donation is complete, it’s important to stay around for at least 10 or 15 minutes. It might be tempting to just leave but this is to ensure that you aren’t lightheaded or feel unwell before you leave and go about your day. Look for the refreshments, usually juice, coffee, tea, cookies, or donuts!
When the blood donation is complete, it’s important to stay around for at least 10 or 15 minutes. It might be tempting to just leave but this is to ensure that you aren’t lightheaded or feel unwell before you leave and go about your day. Look for the refreshments, usually juice, coffee, tea, cookies, or donuts!
After donating a pint of blood you may feel tired. Although your body quickly regenerates plasma and platelets within a few days – your body needs weeks to make new red blood cells. So avoid heavy exercise or alcohol use as you may notice your energy level and tolerance are lower.
Most donation centers recommend 8 weeks between whole blood donations. In some areas, you can donate platelets more frequently (up to every week, but no more than 24 times in a year).
What happens to your blood
After donating, your blood will be checked for certain infectious diseases such as HIV and hepatitis.
Your donation is usually separated into different components. Each can help a different person:
Red blood cells are what you might typically imagine to be a blood transfusion. Patients who might get them are those who need to replace lost blood, maybe from an accident or surgery, or are anemic from chemotherapy. They make up 45% of a pint of blood. Red blood cells can last up to 45 days (refrigerated) from the date of donation.
Plasma, which makes up more than half your blood and is a yellowish or straw-colored fluid extracted from the blood. Donors can give just plasma under a slightly different process– you can learn more about that here. Plasma contains critical proteins that do things like help your blood clot and carry nutrients to your body’s tissues. Patients who might receive plasma are those who have serious immune deficiencies, or autoimmune diseases such as myasthenia gravis. Others include those who have severe liver disease, difficulty clotting their blood, or inherited deficiencies like alpha-1 antitripsin deficiency. Fresh frozen plasma can last up to a year after donation.
Cryoprecipitate is a concentrated component of plasma rich in certain clotting factors. People with hemophilia may receive a cryoprecipitate transfusion to help them clot their blood after an injury. Frozen cryoprecipitate lasts for one year.
Platelets are foro people whose blood doesn’t clot properly, such as those with cancer whose bone marrow isn’t making enough platelets, or whose body is destroying their platelets. This can happen in a rare disorder in pregnant women called HELLP syndrome. Platelets last in a refrigerator for only 5 days due to difficulties with clumping. Organ recipients and heart surgery patients often receive platelets during surgery. You can donate platelets alone every 7 days for up to 24 times a year. However, donating platelets takes about 90 minutes and involves a slightly different process.
According to Cedars-Sinai Medical Center, there is a blood transfusion in the United States every 2 seconds. And 1 in every 7 hospitalized patients requires a blood transfusion. So why should you give? Why not help a friend in need who is going through chemotherapy or requires regular transfusions due to a chronic illness? Maybe you received a blood transfusion after a car accident? Or maybe you want to serve as a good example to family and friends about the importance of community and collaboration.
There is no current viable alternative for blood products. And only 10% of eligible donors currently donate blood. Donated blood is a gift, and it’s one that you or someone you love may need at some time. So, find a local blood drive, save a life and donate today!
Disclaimer
The information in this blog is provided as an information and educational resource only. It is not to be used or relied upon for diagnostic or treatment purposes.
The blog does not represent or guarantee that its information is applicable to a specific patient’s care or treatment. The educational content in this blog is not to be interpreted as medical advice from any of the authors or contributors. It is not to be used as a substitute for treatment or advice from a practicing physician or other healthcare professional.




